
Testicular cancer occurs when abnormal cells develop in the testicles, the male reproductive glands responsible for producing sperm and testosterone. While relatively rare compared to other cancers, it is the most common cancer in men aged 15 to 35. With early detection and treatment, testicular cancer has a high cure rate, even when it has spread beyond the testicle.
Symptoms of Testicular Cancer
Many cases are discovered incidentally during self-examination or routine physical exams. Symptoms may include:
- A painless lump or swelling in one testicle
- A feeling of heaviness or aching in the scrotum or lower abdomen
- Sudden fluid collection in the scrotum
- Dull pain in the back or groin
- Enlargement or tenderness of breast tissue (in rare cases)
Men are encouraged to perform regular testicular self-exams to identify any unusual changes early.
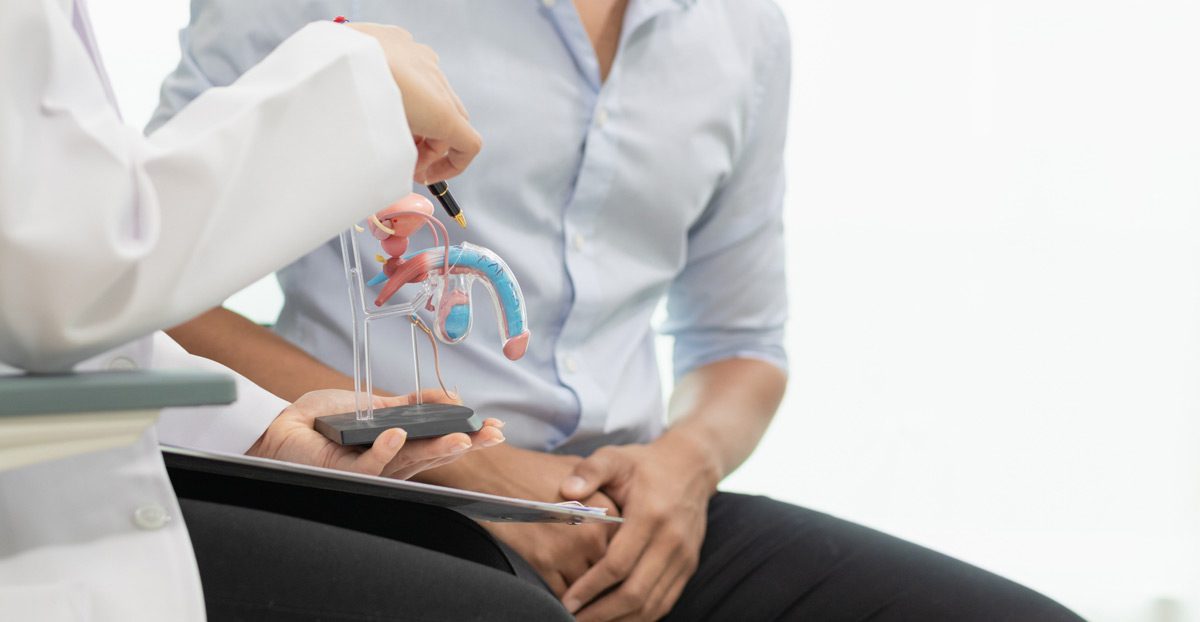
Types and Risk Factors
Most testicular cancers begin in germ cells, which develop into sperm. There are two main types:
- Seminomas: Tend to grow slowly and respond well to radiation
- Non-seminomas: More aggressive but still highly treatable
Risk factors include:
- Undescended testicle (cryptorchidism)
- Family history of testicular cancer
- Personal history of testicular cancer
- Abnormal testicular development (e.g., Klinefelter syndrome)
- Age and race: Most common in young white men
Diagnosis
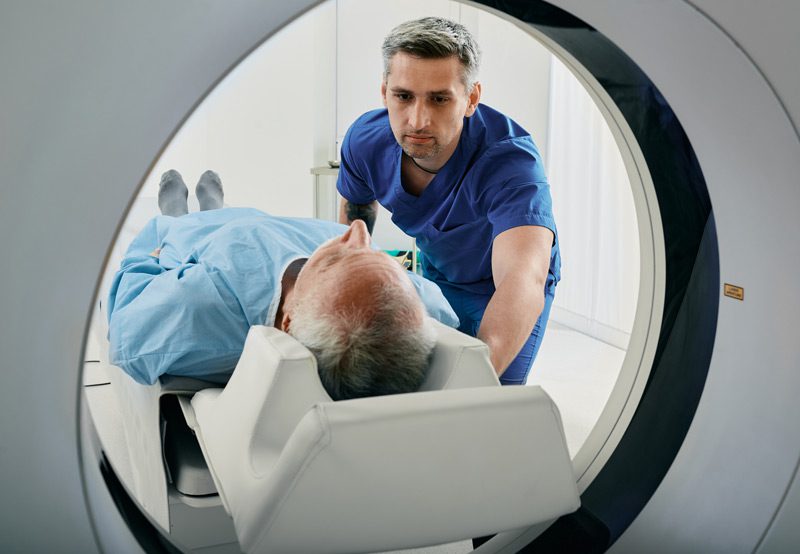
Diagnosis typically begins with a physical exam and ultrasound of the scrotum. Blood tests for tumor markers, such as alpha-fetoprotein (AFP), beta-HCG, and LDH, help identify cancer type and monitor treatment. A CT scan or MRI may be used to evaluate whether the cancer has spread.
Unlike many cancers, biopsy is not performed prior to surgery due to the risk of spreading cancer cells. Instead, radical inguinal orchiectomy (surgical removal of the affected testicle) is performed both to confirm the diagnosis and begin treatment.
Treatment Options
Treatment is based on the type and stage of the cancer:
- Radical Orchiectomy: Removal of the affected testicle is the primary treatment
- Surveillance: For low-risk, early-stage cases with no spread
- Chemotherapy: Often used for advanced-stage or non-seminoma cancers
- Radiation Therapy: Primarily for seminomas
- Retroperitoneal Lymph Node Dissection (RPLND): Surgical removal of lymph nodes in certain cases
Treatment success is high, with cure rates exceeding 95% for early-stage cancer and 70–90% even in metastatic cases.
Follow-Up and Fertility Considerations
Ongoing follow-up includes tumor marker blood tests, imaging studies, and physical exams to detect recurrence. Many men retain fertility after treatment, but those undergoing chemotherapy or RPLND may be advised to bank sperm beforehand.
Support and Outlook
The emotional impact of testicular cancer, particularly in young men, can be significant. Support groups, counseling, and survivorship care are important components of recovery. With prompt treatment, most men return to normal activities and experience long-term remission.
